What You Should Know:
– Value-based care (VBC) has been established as a precedence amongst healthcare organizations and payers as contributors have gained extra expertise in managing their high quality metrics and contracts, finally realizing returns on their investments.
– For their newest report, Value-Based Care Reimbursement 2022, KLAS talked to 54 healthcare executives—together with CEOs, CFOs, CIOs, CMIOs, COOs, VPs and administrators of population health, and VPs of analytics—to gauge how they’re transferring past pay-for-performance into risk-bearing contracts over the following three years and their perceptions on which distributors might help them obtain their upcoming objectives with VBC.
Key Themes and Ideas Regarding Value-Based Care Reimbursement 2022
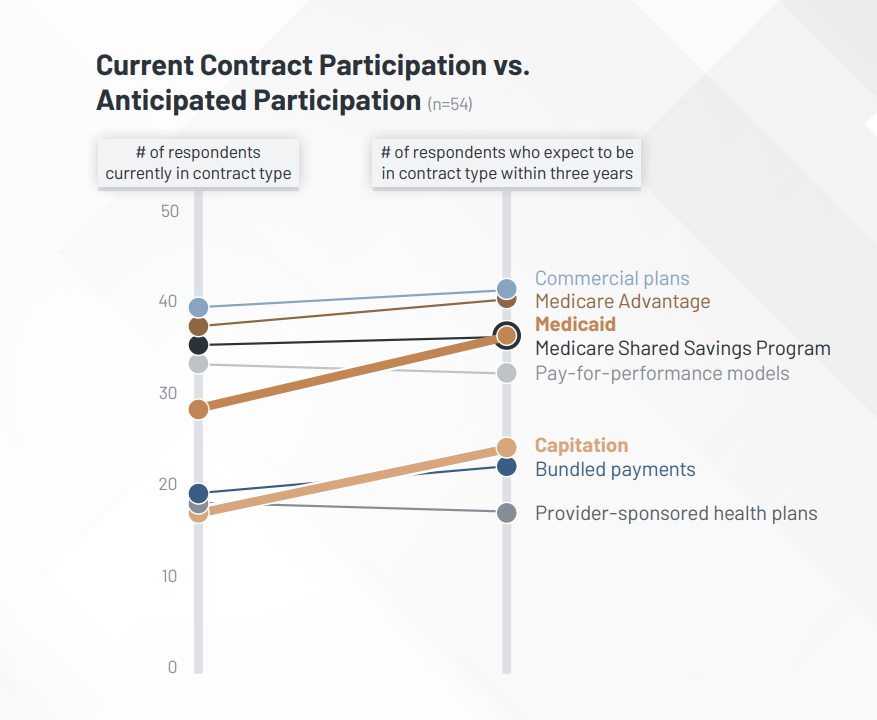
1. Significant Growth Anticipated for Medicaid and Capitation Contracts: Most respondents report strategic plans to develop their VBC contracts over the following three years. Participation in industrial plans, Medicare Advantage, and Medicare Shared Savings Programs will proceed to be excessive, whereas Medicaid plans—which have the potential to influence a big quantity of lives—will see the most important progress. The administration of capitation contracts might be difficult for many who don’t have expertise with them, however they’re rising in attraction, as they permit for extra predictable income than conventional fee-for-service fashions do.
2. Percent of Revenue Tied to VBC Varies Widely: VBC is making headway, however the depth of its adoption varies throughout organizations. Some hospitals are simply beginning out and have little to no income from VBC contracts. On the opposite hand, ACOs and clinically built-in networks, amongst others, could obtain most or all of their income from value-based reimbursement, they usually characterize all organizations in this pattern with over 90% of their income tied to VBC. Nationally, the typical share of income tied to VBC contracts is about 10%. Even amongst this report’s pattern, which consists principally of extra progressive organizations, 50% obtain one-fifth or much less of their income from value-based reimbursement.
3. Respondents Overwhelmingly Expect to Bring in More Revenue from VBC in the Future: A overwhelming majority of respondents anticipate {that a} bigger share of their income shall be tied to VBC three years from now. Key drivers of that expectation are newly out there alternatives for VBC contracts and market pressures from payers and the federal government as they transfer the business in the route of VBC.
4. Provider Organizations Are Consolidating Their VBC Vendors: Overall, supplier organizations are lowering the quantity of know-how distributors or providers companies they use to assist VBC.† Only 20% of respondents use greater than two distributors to assist them deal with VBC; wanting a one-stop store for knowledge aggregation, analytics, and reporting, the bulk have consolidated to both one or two.
5. Epic, Arcadia, and Innovaccer Seen as Most Able to Assist Organizations with Future VBC Needs: Epic’s broad buyer base feels that the seller will be capable to help them with their future VBC wants resulting from enhancements Epic is making to Healthy Planet. Respondents additionally acknowledge the benefit of Healthy Planet being in the suppliers’ day-to-day workflow, as it’s built-in with the primary Epic medical report. Respondents notice that Arcadia will be capable to present for future wants as a result of they provide a full suite of merchandise, together with strong knowledge aggregation, reporting, and AI coding capabilities. Additionally, respondents spotlight Arcadia’s potential to shut high quality gaps and examine each medical and monetary knowledge in one report. Likewise, respondents spotlight Innovaccer as a vendor that can be capable to help with VBC in the long run as a result of of their spectacular dashboards and predictive analytics. Additionally, Innovaccer is reportedly keen to construct custom-made options to fulfill prospects’ distinctive wants.
“If we determine we wish to hyperlink extra strong govt dashboards to trace our efficiency with value-based care as we get larger and we want higher dashboards than what we will get from Epic or our present vendor, we may have the product. We are high-quality now, however as we develop, we may have higher dashboards. I’ve seen Arcadia’s govt monitoring dashboards, they usually look phenomenal. The product could be a alternative. I might use Arcadia’s predictive analytics as nicely as a result of they’re pretty much as good as, if not higher than, what we now have.” —VP of inhabitants well being
https://information.google.com/__i/rss/rd/articles/CBMiSWh0dHBzOi8vaGl0Y29uc3VsdGFudC5uZXQvMjAyMi8xMS8zMC9rbGFzLXZhbHVlLWJhc2VkLWNhcmUtcmVpbWJ1cnNlbWVudC_SAQA?oc=5






